
Manufacturing Safe Vaccines
The coronavirus pandemic has transformed 2020 into one of the most challenging years in recent memory, disrupting our lives in ways big and small. As infection rates around the world have continued to fluctuate, the medical and scientific communities have worked overtime to understand how the disease is transmitted, how to treat those who become infected, and how to prevent people from getting it in the first place. This is where vaccines come in.
The unusual speed with which the various coronavirus vaccine candidates have been developed, coupled with the circulation of misinformation regarding alleged side effects, have led a certain percentage of the population to re-evalueate their interest in a COVID-19 vaccine. Researchers refer to this problem as “vaccine hesitancy.”
For instance, a survey of over 13,000 people in 19 countries conducted last June by the publication Nature Medicine reported that 71.5% of participants would be likely or somewhat likely to take a COVID-19 vaccine. Looked at from the opposite perspective, however, that means nearly 30% of respondents either expressed no opinion (14.2%) or were somewhat (6.1%) or completely (8.1%) unlikely to accept a vaccine.
READ MORE: 5 Essential Standards for Pharmaceutical Manufacturing
Against this backdrop, it’s even more important for the pharmaceutical companies that are making these vaccines to follow widely accepted and broadly used product purity and process sterility standards. To that end, the committee on manufacture of pharmaceutical and biopharmaceutical products (E55) and its various subcommittees are developing new strategies, test methods, and standard guides as well as updating existing ones that address issues related to vaccine production.
The resulting standards will be applicable to manufacturing processes used for a variety of pharmaceutical products. Of the highest interest, given the ongoing pandemic, are the vaccines developed to combat COVID-19.
Protection and Prevention
ASTM is no stranger to the complex issues faced by medical professionals who deal with infectious diseases. Many ASTM standards covering masks, gowns, gloves, and hand sanitizers have been published and are in use today. ASTM International continues to provide no-cost public access to 27 such standards to support manufacturers, test labs, healthcare workers, and the general public in the fight against COVID-19 (see www.astm.org/COVID-19).
Masks, gloves, and other forms of personal protective equipment are designed to serve as barriers against airborne germs and contaminated surfaces. Think of this as an approach to disease spread at the “macro” level, in hospitals and other healthcare delivery locations where the presence of sick people makes it difficult or even impossible to avoid contact with dangerous microorganisms and viruses.
Facilities where pharmaceuticals and biopharmaceuticals are manufactured, on the other hand, operate at more of a “micro” level. Their goal is to establish a highly controlled environment that is classified for air quality (according to standards from the International Organization for Standardization, ISO) and provides a high assurance of sterility. To do so requires eliminating, or minimizing to the greatest extent possible, the presence of potential microbiological contaminants in order to ensure the safety of vaccines and other medications.
Industry consultant Duncan Low, an E55 member, cites bacteria, fungi, and viruses as examples of single-celled microorganisms that can compromise a vaccine. He explains that these contaminants can originate from various sources, including both production inputs such as animal-sourced raw materials (enzymes, sera) and the surrounding environment — for example, airborne contamination from personnel, rodents, and insects. “Contamination of a vaccine could result in a variety of negative effects, from loss of efficacy up to and including disease or fatal side effects for a patient,” says Low.
E55’s subcommittees have developed various standards that help manufacturers by providing best practices for handling and producing pharmaceuticals. Inventory control of biological materials, integrity testing and assurance of single-use systems, and science- and risk-based cleaning process development and validation are just a few examples, as is an update to a key filtration standard that has been in use for decades.
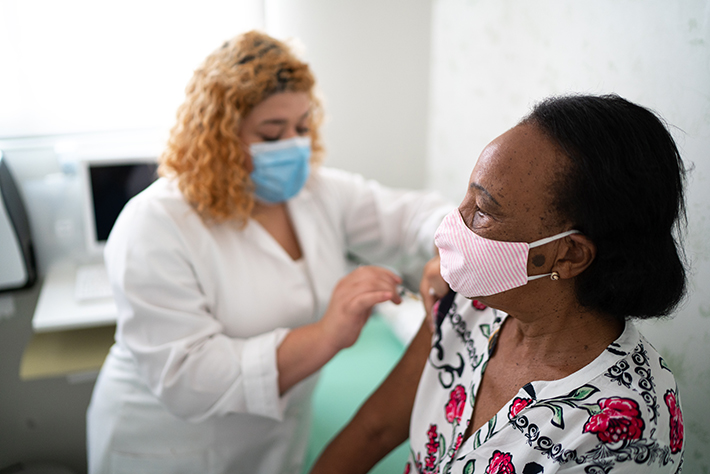 COVID-19 vaccines are being rolled out across the U.S. and around the world.
COVID-19 vaccines are being rolled out across the U.S. and around the world.
Focus on Membrane Filters
The primary objective of achieving sterility in pharmaceutical manufacturing is to prevent bacteria and other microbiological contaminants from infiltrating the production process. One of the latest accomplishments of the subcommittee on general pharmaceutical standards (E55.03) — one with a direct impact on vaccine production — is the recent approval of revisions to a membrane filter standard.
The test method for determining bacterial retention of membrane filters utilized for liquid filtration (F838) helps determine the efficacy under standardized conditions for this type of filter. First published in 1983, the test is widely referenced in the industry. “F838 is used internationally by filter companies and pharmaceutical and biopharmaceutical manufacturers as the basis for claiming that a microporous membrane filter is capable
of producing a sterile filtrate under the conditions specified in the standard,” says Russell Madsen, who is president of The Williamsburg Group, a pharma industry consulting firm, and an E55.03 member.
According to Madsen, F838 is loosely based on the work of Frances Bowman, a U.S. Food and Drug Administration (FDA) scientist. In 1960, she discovered that 0.45 micron-rated microporous membrane filters would pass small microorganisms (B. diminuta) if they were present at levels above 104–106 per cm2 effective filter area. Her findings revealed the need for a test that could determine the ability of these filters to reliably remove microorganisms from a pharmaceutical product during a sterilizing filtration process. This work eventually led to the publication of the ASTM International standard.
While the changes to F838 approved last September were largely editorial in nature, they nonetheless provide important clarification in several key areas. “The updates involved Figure 1 and Section 13, the Test Procedure,” Madsen says. “In previous versions of the standard, there were discrepancies between the figure and test procedure in terms of nomenclature. For example, the test procedure used different designations for the test analysis and control analysis filters shown in Figure 1. The stakeholders rightly wanted to remove ambiguity from this important standard.”
Madsen also notes additional changes to the test method that focus on proper formatting of SI units — the world’s most widely recognized system of measurement — referenced in the standard. “The last iteration of the standard was approved by the committee and subcommittee in September 2020 after extensive review and updating by subject matter experts representing filter users, filter manufacturers, and the FDA,” he says.
Three New Standards
Three standards are now under discussion within the subcommittee on microbial/sterility assurance for pharmaceutical and biopharmaceutical products (E55.06).
Active since December 2018, this subcommittee was formed to support industry efforts in the area of microbiological quality and to ensure that this critical requirement is addressed by other E55 published and draft standards.
FOR YOU: The 10 Most Read Features of 2020
The goal of the subcommittee is to improve standardization for the microbiological quality of pharmaceutical and biopharmaceutical products. One of the key aspects of E55.06’s work focuses on the purity of the microbiological components that are the building blocks of many modern vaccines.
Sterility is an example of just how complex the issues faced by this subcommittee can be. Many products, vaccines included, require the final product be sterile. However, the term “sterile” is very narrow and does not always reflect today’s product challenges.
Therefore, standards that support the highest possible assurance of sterility are relevant to every category of pharmaceutical products, regardless of how they are made.
The good news is that E55.06 is on the case. And the subcommittee’s recent work on the Microbial Contamination Prevention Strategy in the form of WK69660 aims to assist firms when developing a comprehensive program for microbial contamination control. This begins with sourcing appropriate materials and tools to control and monitor microbial quality.
Airflow and Gowning
Two other initiatives are also under way within this subcommittee. One focuses on airflow in cleanrooms, the other on the clothing individuals wear when working in such environments.
ISO 14644 describes the use of a smoke study as a tool. However, there is not a great deal of guidance on how an airflow visualization study should be performed, and the subcommittee plans to provide guidance on best practices in this area. In particular, computational fluid dynamic studies could play a big role.
Gowns represent another element of the microbiological quality equation. Choosing the proper type of cleanroom apparel is an important decision that should take into account how the particular attributes of a given garment match up with the needs of the production process.
Cell-therapy production processes may require sterile gowns that protect the process but that also offer biohazard protection for the operator. The goal of future work in this area, like other committee initiatives, is to provide users with guidance, in this case in the selection of cleanroom apparel.
Leveraging Global Connections
Although the committee on manufacture of pharmaceutical and biopharmaceutical products and its subcommittees have been grappling with issues of pharmaceutical quality since well before the arrival of COVID-19, the pandemic has added a new sense of urgency to their efforts, and it has reinforced the importance of international cooperation and coordination when dealing with a global health crisis.
Among the key challenges faced by those in the standards development community is the unprecedented speed with which vaccines may need to be developed.
And in the complicated environment surrounding the sprint toward a COVID-19 vaccine, a consensus-based approach to quality standards, backed by data and based on input from experts representing different relevant disciplines, should help reassure the world about the safety of a vaccine. ■
Jack Maxwell is a freelance writer based in Westmont, New Jersey.
 SN Home
SN Home Archive
Archive Advertisers
Advertisers Masthead
Masthead RateCard
RateCard Subscribe
Subscribe Email Editor
Email Editor