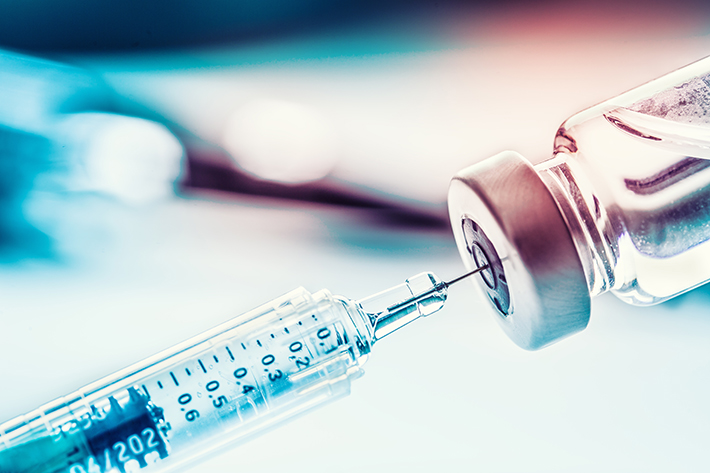
The Right Combination
Combination products, generally speaking, pair drugs with a delivery system to treat many and diverse medical conditions and illnesses. There are many different types of combination products, but the understanding of these medicines varies from one country to another, and many still lack guidance or regulations.
To change that situation, a group has begun related work in the committee on manufacture of pharmaceutical and biopharmaceutical products (E55). Under the subcommittee on general pharmaceutical standards (E55.03), representatives of pharma corporations, government health agencies, medical consultancies, and more aim to support all those involved, and ultimately, patients and their health. Their first proposed standard: a guide to define and give examples of combination products, with others to follow.
Toward Definitions
“I think that globally, regulatory frameworks are working to drive successful practices and control strategies throughout the combination product lifecycle to assure public health,” Susan Neadle says. “The challenge we are all facing, however, is that combination product terminology and definitions are not aligned across jurisdictions, and that leads to confusion.”
FOR YOU: 5 Essential Standards for Pharmaceutical Manufacturing
Neadle is part of the E55 group that is defining and characterizing combination products. As senior director, global value chain quality design, she heads up a Johnson & Johnson community of practice with people who are working on combination products across consumer products, medical devices, and pharmaceuticals, and she has extensive experience in the field.
“The regulatory pathway that a combination product follows is driven by its primary mode of action,” Neadle explains. “But there are different interpretations globally, and a product that is considered a medicine in one country might be considered a medical device in another. That means there are different requirements that companies have to live up to, both during development and for lifecycle management.”
Think of a stent. It’s a device to open an artery or vein that is also impregnated with a medicine to keep that opening in place. Or consider an inhaler, which has contents to help ease breathing; it needs both the medication and the targeted delivery system. Or take an epi-pen, which puts the drug and the injector into one ready-to-use assembly.
Combination products typically use bioproteins that have a significantly larger molecular weight than an antibiotic or over-the-counter tablet such as aspirin or a liquid also taken orally. A bioprotein, which often degrades quickly, needs to reach the targeted site and provide relief or healing. Such drugs need to be injected, for example, as with a multiple sclerosis treatment, or need to be infused to reach a site quickly and accurately, as with cancer drugs. Some need to be implanted, as with the aforementioned stent.
“Combination products are the way of the future,” says Ferdinando Aspesi, Ph.D., chair of the ASTM International pharma/biopharma committee and senior partner at Bridge Associates International, which provides manufacturing and quality-related services to the pharmaceutical industry.
Manfred Maeder, Ph.D., concurs: “More than 50% of submissions have been biologics recently. Combination products are the only tool to get the medication into the body [e.g., syringe, autoinjector, or pump], therefore, a CP is not a benefit, but rather, the only possible tool,” he says. Maeder is global head of device development and commercialization for Novartis, and he leads the task group working on the proposed standard.

The asthma inhaler is one of the most well known combination products in the world.
And consider that studies vary as to predictions about how much the market for combination products will expand over the next 4 or 5 years. One study indicates the market value will be $177.7 billion USD and another $164.7 billion USD. These different numbers may also provide a clue about the differences in understanding what a combination product can be.
Similarities and Differences
Combination products date back to 1914, Neadle says. “The original hypodermic syringe patent was issued to Rob Porter in 1914, decades after subcutaneous and intramuscular drug delivery was performed using a glass vial and hypodermic syringe,” she notes. However, technology and treatment came together on behalf of patients much more recently, in the 1970s and 1980s, with advances like pre-filled insulin pen injectors.
In the United States, the founding of the Food and Drug Administration’s Office of Combination Products was still a few decades away, occurring in 2002. Today, this office is represented on the E55 group. The United Kingdom’s MHRA (Medicines and Healthcare Products Regulatory Agency) and the EMA (European Medicines Agency)are also participating in the group, along with representatives of pharmaceutical companies.
Maeder points out another example of the ways countries vary on the definition of combination products, with differences between Canada and the United States. Both countries use these two definitions for combination products: A “single entity” combination product comprises two or more regulated components, while “co-packed” combination products are two or more separate products — drug and device, or device and biological — packaged together. Canada, however, does not use the third U.S. type: “cross-labeled” combination products, which involve separate packages intended to be used together.
And that’s just one example. Another is the fact that the European Medicines Agency has no formal legal definition for combination products but rather issues guidance that categorizes combination products differently than in the United States.
Overall, as Maeder notes, “The vast number of countries have no definition for a combination product.”
Whatever the submission requirements are, Aspesi summarizes the issue this way. “If you don’t have a good definition of what you are talking about, then the work to get approvals ultimately is difficult.”
Beyond Definitions
The work to define and harmonize combination product definitions is just the starting point for the E55 group. Other standards will follow, and there’s a broad range of possibilities.
READ MORE: Pharmaceuticals Get Smart
“Health authorities globally are working to ensure that the regulatory frameworks and the quality management system are right,” explains Neadle. “They want to make sure that the biologics and the cell-tissue therapies available are safe and effective, and they want to make sure the devices used stay safe.”
For example, then, standards could apply across a product lifespan. Aspesi says, “You need to make sure the development of the product, as well as the delivery system of the product, are properly evaluated.” That includes human factors such as ease of use and possible misuse.
That also applies to the materials used to produce the delivery systems, such as the plastics and metals in a syringe, to ensure that the device has the strength to work properly and doesn’t leak. It applies to ensuring that the medicine won’t be affected by its container (no leaching or other contamination) and end up in the patient’s body. And new materials must be tested for how they will be used.
The possibilities for standards could also include how combination products are labeled. What patient considerations need to be addressed, such as type legibility?
In addition, Aspesi notes that a world of connectivity should be considered. Perhaps the combination product includes a sensor to check a patient’s blood sugar, for example, and the data may be recorded somehow. How do you ensure that the data is secure? If the data gets transmitted to a doctor or to an online repository, how is that stored accurately and securely? The information itself must be considered, as must the software.
Take that a step further, to digital health overall. “Digital technologies and product delivery and compliance functions are in their infancy, but growing fast. It would be great if we could align strategies to ensure the relevance, safety, and efficacy of this new class of products to help build a framework effectively,” says Neadle.
Neadle also wonders if there could be a “Master File” strategy for the constituent parts that comprise combination products, to support risk-based approaches and efficiencies in development and review of these products. She also sees usefulness in standards to guide required combination product post-market safety reporting. Expanding on the varied expectations and regulatory pre-market pathways, this process further compounds the complexity due to reporting differences around the world.
“There’s no shortage of opportunities,” Neadle summarizes. “It’s a matter of prioritizing where we want to go.” ■
 SN Home
SN Home Archive
Archive Advertisers
Advertisers Masthead
Masthead RateCard
RateCard Subscribe
Subscribe Email Editor
Email Editor